 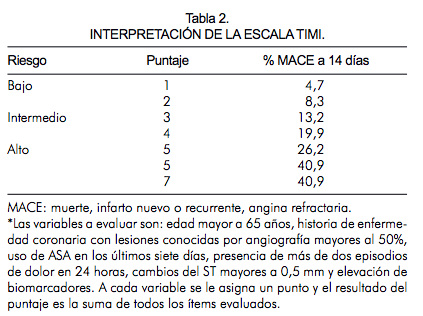
By incorporating events during the index hospitalization, it can better define risk and help to guide treatment decisions. This score is a prospectively derived, validated means of estimating 1-year mortality of STEMI at hospital discharge and can serve as a clinically useful tool. In the validation database, the C-statistic was 0.81, with a NRI of 0.35 (P=0.01). The C-statistic produced by the dynamic score in the derivation database was 0.76, with a net reclassification improvement (NRI) of 0.33 (P<0.0001) from the inclusion of dynamic events to the original TIMI risk score. The dynamic score included the development of in-hospital MI, arrhythmia, major bleed, stroke, congestive heart failure, recurrent ischemia, and renal failure. Each variable was assigned an integer value based on the odds ratio, and the final score was the sum of these values. Variables with P<0.05 were incorporated into a full multivariable Cox model to assess the risk of death at 1 year. Each variable was tested individually in a univariate Cox proportional hazards regression. New variables were major clinical events occurring during the index hospitalization. Baseline variables were from the original TIMI risk score for STEMI. The dynamic TIMI risk score for STEMI was derived in ExTRACT-TIMI 25 and validated in TRITON-TIMI 38. A dynamic risk score provides an initial risk stratification and reassessment at discharge. They note the need for future studies to validate this model and if the “model stands up to widespread validation in non-trial cohorts, it could be incorporated in future guidelines to guide the care of patients with diabetes.Although there are multiple methods of risk stratification for ST-elevation myocardial infarction (STEMI), this study presents a prospectively validated method for reclassification of patients based on in-hospital events. Eagle, MD, MACC, write that it is important to acknowledge the studies limitations, including the generalizability because only 35% of the study cohort was women and only 20% were non-White. In an accompanying editorial comment, Kent Brummel, MD, and Kim A. The authors write they developed and externally validated a diabetes-specific risk model for predicting atherothrombotic events in patients with T2D and that it “performs well in patients with and without established ASCVD, demonstrating its value in both primary and secondary prevention, and has the potential to inform clinical decision-making.” Of note, patients with higher predicted baseline risk had a greater absolute reduction in the rates of MI and IS with both dapagliflozin and evolocumab (absolute risk reduction: 2.1% vs. The model was calibrated for both primary and secondary prevention. 
Furthermore, the model identified a greater than eight-fold gradient of MI or IS rates between the top and bottom risk quintiles in the pooled cohort (three-year Kaplan-Meier rate: 14.9% vs. Results found 16 routinely measured variables were independent predictors of MI or IS. They also examined treatment interactions with dapagliflozin and evolocumab using data from the DECLARE-TIMI58 and FOURIER trials, respectively. Berg, MD, MPH, FACC, et al., pooled 42,181 patients with T2D from four trials in the Thrombolysis In Myocardial Infraction (TIMI) program to develop and validate a risk model for myocardial infarction (MI) or ischemic stroke (IS). A newly developed risk model for atherothrombosis in patients with type 2 diabetes (T2D) has the potential to improve risk assessment and better inform clinical decision-making, according to a study published June 19 in JACC.ĭavid D. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
